Weather Allergies in Children: Causes, Symptoms and How Parents Can Help
Weather changes can bring joy — blooming flowers in spring, crisp air in autumn, sunny summer days and cozy winter nights. But for many children, these seasonal shifts also bring something less pleasant: weather allergies. These allergies can cause runny noses, itchy eyes, coughs and skin reactions, making daily life uncomfortable for your child.
This guide will help parents understand the causes, symptoms, prevention, and treatment of weather allergies in children and how to support them through seasonal changes.
1. What Are Weather Allergies in Children?
Weather allergies occur when a child’s immune system overreacts to environmental changes or seasonal triggers, such as:
-
Pollen from trees, grasses and weeds
-
Mold spores that thrive in damp conditions
-
Dust mites more active in certain climates
-
Cold air that dries and irritates airways
-
Rapid temperature changes affecting skin and respiratory health
These reactions are part of allergic rhinitis (hay fever) or skin allergies like eczema flare-ups.
2. Common Causes and Seasonal Triggers
Spring
-
Tree pollen is the biggest trigger.
-
Mold spores increase with rain and humidity.
Summer
-
Grass pollen peaks.
-
Insect stings and bites can trigger allergic responses.
Autumn
-
Weed pollen (ragweed, mugwort).
-
Mold from fallen, damp leaves.
Winter
-
Dust mites and pet dander accumulate indoors.
-
Cold, dry air can cause skin irritation and asthma flare-ups.
3. Signs and Symptoms to Watch For
Respiratory symptoms:
-
Sneezing
-
Runny or stuffy nose
-
Coughing and wheezing
-
Itchy throat
Eye symptoms:
-
Redness
-
Itching
-
Watery discharge
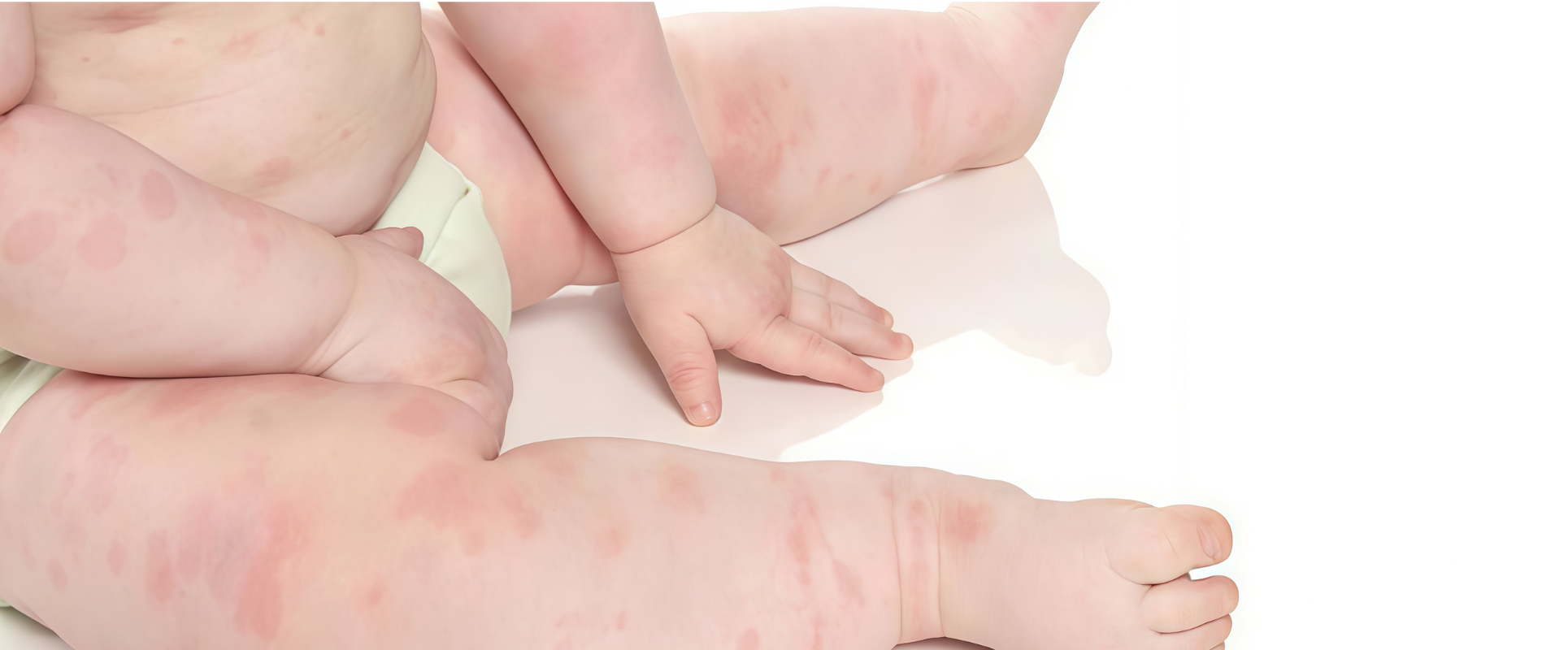
Skin symptoms:
-
Dryness or eczema patches
-
Hives
Behavioral signs in young children:
-
Rubbing eyes or nose frequently
-
Disturbed sleep
-
Irritability
4. How Weather Allergies Differ From a Cold
|
Feature |
Weather Allergy |
Common Cold |
|---|---|---|
|
Cause |
Immune reaction to allergens |
Viral infection |
|
Fever |
Rare |
Common |
|
Onset |
Immediate after allergen exposure |
1–3 days after infection |
|
Duration |
Weeks or months |
7–10 days |
|
Mucus color |
Clear |
Often yellow/green later |
5. Diagnosis
A pediatrician or allergist can confirm weather allergies through:
-
Medical history review
-
Physical examination
-
Allergy skin tests
-
Blood tests for allergen-specific antibodies
6. Treatment Options
Lifestyle and Home Care
-
Keep windows closed during high pollen days.
-
Use air purifiers with HEPA filters.
-
Wash your child’s hair and clothes after outdoor play.
-
Use saline nasal sprays to rinse allergens.
Medical Treatments
(Only under medical supervision)
-
Antihistamines (liquid or chewable)
-
Nasal corticosteroid sprays
-
Eye drops for allergic conjunctivitis
-
Moisturizing creams for skin allergies
7. Prevention Tips for Parents
-
Check daily pollen counts — limit outdoor activities when levels are high.
-
Maintain indoor humidity between 40–50%.
-
Vacuum regularly with a HEPA filter vacuum.
-
Avoid strong perfumes or cleaning chemicals that may worsen allergies.
-
Encourage handwashing after outdoor play.
8. When to Seek Medical Help
Seek urgent care if your child:
-
Has difficulty breathing
-
Experiences swelling of the lips or face
-
Develops severe hives
-
Shows signs of anaphylaxis (call emergency services immediately)
9. Supporting Your Child Emotionally
Allergies can limit activities, making children feel left out. Parents can:
-
Explain what allergies are in a simple way.
-
Plan alternative indoor fun on high-allergen days.
-
Work with teachers to ensure school support.








