Fungal Skin Infections in Children: Causes, Symptoms and Safe Treatments
Fungal skin infections are among the most common childhood skin conditions. They can appear as itchy rashes, red patches or ring-shaped lesions that cause discomfort for children and concern for parents. While not usually dangerous, fungal infections need proper care and hygiene to prevent spreading and recurring.
This blog explores the causes, symptoms, treatment and prevention of fungal skin infections in children. Parents will also find practical tips for protecting sensitive young skin using safe, natural methods.
What Are Fungal Skin Infections in Children?
Fungal infections (also called dermatomycoses) are caused by fungi such as dermatophytes, yeasts or molds that grow on the skin, hair or nails. Children are particularly vulnerable because their skin barrier is still developing and they often share toys, clothing or sports equipment that can spread fungi.
Common types of fungal infections in children:
-
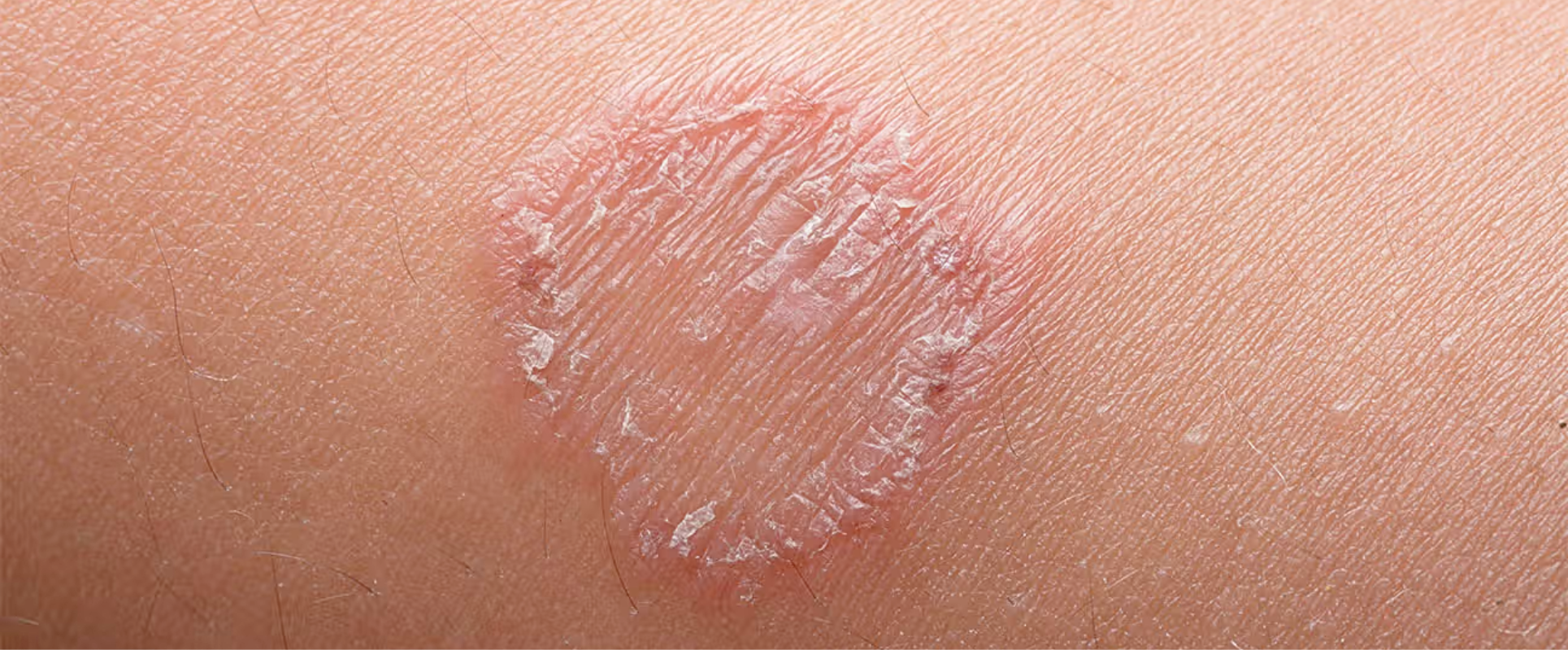
Ringworm (Tinea corporis): Circular, red, scaly patches with a clear center.
-
Athlete’s foot (Tinea pedis): Itchy, cracked skin between the toes.
-
Scalp ringworm (Tinea capitis): Patchy hair loss with scaling on the scalp.
-
Yeast infections (Candida): Often in warm, moist areas like diaper regions or skin folds.
Symptoms Parents Should Watch For
Fungal infections may look similar to other rashes, but key symptoms include:
-
Itchy, red or scaly patches on skin
-
Ring-shaped lesions with raised borders
-
Cracked or peeling skin (especially on feet)
-
White patches in the mouth (oral thrush)
-
Brittle or discolored nails (in nail fungus)
Parents should consult a pediatrician if the rash spreads, causes pain or does not improve with basic care.
Causes and Risk Factors
Children may develop fungal skin infections due to:
-
Warm, humid weather (ideal for fungal growth)
-
Sweating after play or sports activities
-
Shared items like towels, hats or bedding
-
Weakened immunity or recent antibiotic use
-
Poorly ventilated clothing that traps moisture
Diagnosis and When to See a Doctor
Doctors usually diagnose fungal infections through a skin examination and sometimes a microscopic test (KOH test) or culture. Parents should not rely only on home remedies or self-diagnosis since some bacterial rashes may look similar.
Seek medical help if:
-
The infection spreads quickly
-
The child has scalp involvement or hair loss
-
There is fever or swollen lymph nodes
-
Over-the-counter antifungal creams fail after 1–2 weeks
Treatment Options for Children
1. Medical Treatments
-
Topical antifungal creams/ointments (clotrimazole, miconazole, terbinafine) are commonly prescribed.
-
Oral antifungals may be necessary for scalp or nail infections.
-
Steroid creams are not recommended, as they can worsen fungal growth.
2. Natural and Supportive Care
-
Keep the skin clean and dry.
-
Use breathable cotton clothing.
-
Change socks and underwear daily.
-
Choose gentle, natural skincare products that do not irritate sensitive skin.
For parents seeking safe care, DabiDabi products—made from natural plant-based ingredients and free from alcohol—help keep children’s skin clean, soft and protected.
Prevention Tips for Parents
Prevention is key to reducing fungal infections in children. Practical tips include:
-
Teach children to wash hands and feet daily.
-
Avoid sharing hats, hairbrushes or towels.
-
Keep children’s nails short and clean.
-
Use antifungal powders if children are prone to sweaty feet.
-
Disinfect toys and sports equipment regularly.
-
Strengthen immunity through balanced nutrition and outdoor play.
Complications if Left Untreated
Although most fungal infections are mild, untreated cases may cause:
-
Spread to other areas of the body
-
Secondary bacterial infections from scratching
-
Hair loss and scarring (in scalp infections)
-
Chronic or recurrent rashes
Timely treatment and preventive care help avoid these complications.
Final Thoughts
Fungal skin infections in children are common but manageable. With proper hygiene, safe skincare and timely medical support, parents can protect their child’s skin from discomfort and recurrence.








